
| Overview: women’s health across life stages
Women’s health is rarely defined by a single symptom, a single system, or a single season of life. A woman may be dealing with fatigue, sleep disruption, painful periods, brain fog, pelvic discomfort, autoimmune symptoms, or a persistent sense that something in her body is no longer functioning the way it once did. Beneath those symptoms, there is often a broader pattern involving stress, nervous system strain, inflammation, hormonal shifts, scar tissue, and the body’s ability to recover. As women move through puberty, pregnancy, postpartum recovery, perimenopause, and menopause, their bodies are continually adapting. That is why meaningful healing often requires a wider lens, one that looks beyond isolated symptoms and considers how these systems influence one another over time. Key ideas to keep in mind:
In the sections below, we explore why many women feel dismissed, how stress and hormones interact, how fascia and scar tissue can shape healing, and where to begin when the body feels overwhelmed. |
How women’s health is often reduced to separate symptoms
Much of conventional care is built around a sick-care model. It is designed to respond when something is clearly wrong, diagnose the immediate issue, and manage the symptom in front of the provider. That can be important, especially in acute situations, but it does not always serve women well when symptoms are layered, chronic, or difficult to explain.
Poor sleep, pain, inflammation, nervous system strain, hormone changes, and tissue restriction often overlap. They influence one another quietly, then accumulate over time. When each symptom is treated as a separate problem, the deeper pattern can be missed.
This is one reason so many women in pain feel like they are getting partial answers. One issue may be labeled hormonal. Another may be attributed to stress. Another may be brushed aside as part of aging, motherhood, or a busy season of life. Meanwhile, the body is still asking for support at the root.
A well-care model takes a wider view. Instead of waiting for the body to break down, it asks what conditions may be making healing harder in the first place. Across puberty, pregnancy, postpartum recovery, perimenopause, and menopause, women’s symptoms often reflect an ongoing relationship between the nervous system, hormones, connective tissue, inflammation, and recovery capacity.
When that relationship becomes strained, the body does not always fail dramatically. Sometimes it simply becomes harder to feel steady, rested, resilient, or at home within yourself.
Why a whole-body approach matters in women’s health
When symptoms are treated one at a time, like in the sick-care model outlined above, it can be easy to miss how closely connected they really are. Stress can affect hormones. Hormonal shifts can disrupt sleep. Poor sleep can increase inflammation. Over time, these patterns can reinforce one another in ways that are easy to miss when symptoms are viewed in isolation.
This is what that connection can look like in practice.
How it’s all connected
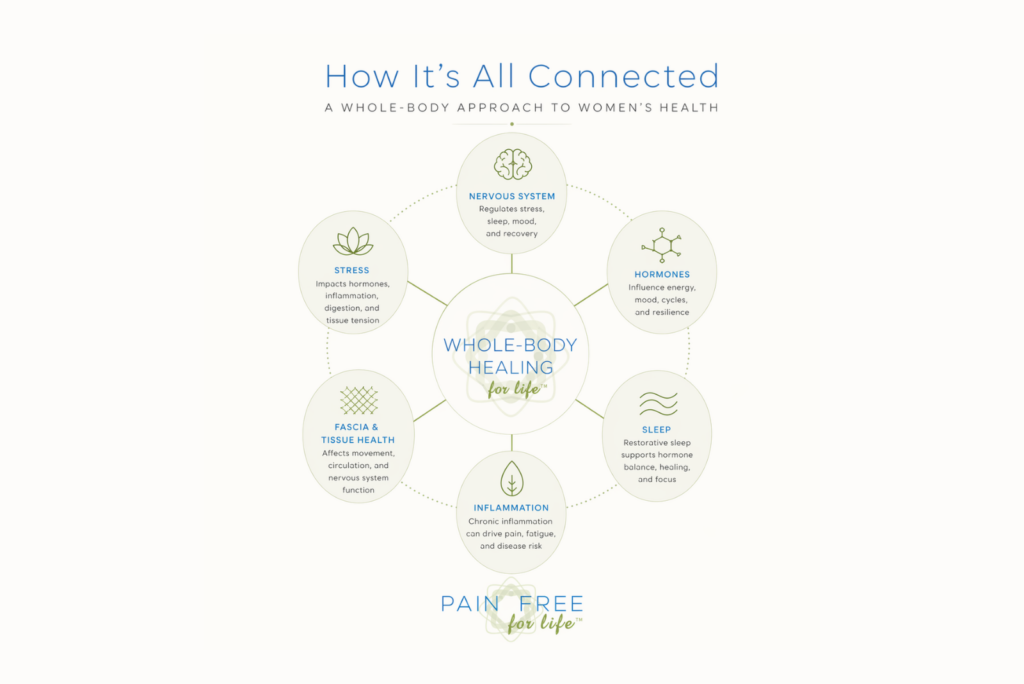
When we talk with women in the Pain Free For Life support group, we often hear a similar thread:
“I knew something was off, but I didn’t know where to start.”
“I thought I just had to keep going.”
“I didn’t realize how long I had been functioning in survival mode.”
Many women are not pushing through chronic pain, fatigue, or inflammation because it does not matter. More often, they are trying to keep up with the constant demands of daily life while their bodies keep asking for support in quieter ways. Over time, it can become normal to function while exhausted, overstimulated, and increasingly disconnected from what the body has been trying to communicate.
In a recent Pain Free For Life roundtable, Care Team members Andrea, Robin, and Annie joined Dr. Rob Vanbergen to explore the patterns they see most often in their own lives and in the women they support. Their conversation touched on sleep, vagus nerve support, hormone-related symptoms, chronic stress, fascia restrictions, and the hidden cost of carrying too much for too long.
Watch below to hear insights from our female-forward Care Team.
Why self-care matters in women’s health across life stages
One of the clearest messages from the conversation in the featured video above is that women’s health often requires permission to be taken seriously before it can be properly supported.
Many women are used to caring for everyone around them while placing their own needs further down the list. Over time, that pattern can make exhaustion, pain, inflammation, poor sleep, or emotional overwhelm feel normal, even when the body has been asking for support for a long time.
Self-care, in this context, is not about indulgence or escape. It is about restoring the basic conditions the body needs in order to function, repair, and communicate clearly. When a woman is depleted, inflamed, anxious, or running on empty, it becomes much harder to show up fully for the people and responsibilities that matter to her.
Supporting your health is not separate from caring for your family, your work, or your future. It is one way you make that care more sustainable.
Why do so many women feel dismissed in healthcare?
Many women recognize that something is changing in their bodies long before they have language for it.
They notice that their energy is less stable. Their periods become more painful. Their sleep grows lighter. Their mood becomes less predictable. Their body feels puffy, inflamed, heavy, or tense in ways that are difficult to explain. Yet too often, these shifts are minimized as normal, attributed only to stress, or folded into vague reassurances about aging. That pattern is part of what we have written about before in Are Your Pain Management Doctors Giving You “Doc Block”?, where the deeper issue is not just delay, but the way women’s symptoms are too often filtered through assumptions before they are fully investigated.
The cost of that dismissal can be significant. According to the Organization for Autism Research, only 20% of girls with autism are diagnosed before age 11, compared with 50% of boys. In fact, Michigan State’s Women’s Health Research Institute highlights that more than 40% of women eventually diagnosed with a serious autoimmune disease had previously been told they were overly concerned or hypochondriacs.

That dismissal creates its own kind of strain. A woman feels that her body is asking for support, but begins to question her own perception because the answers she receives are often too narrow, too rushed, or too fragmented to account for what she is actually experiencing.
This is one reason a whole-system approach matters. Hormones affect sleep. Stress influences digestion. Scar tissue can alter mobility and posture. Nervous system overload can shape everything from inflammation to pain tolerance. When symptoms are viewed in isolation, important connections are missed.
A timely opportunity to learn more about women’s health

The Women’s Health Rescue Summit is premiering free May 11–17, 2026, bringing together more than 35 doctors, researchers, and clinicians focused on women’s health. The goal is to make research-backed information easier to understand and more useful in real life.
Dr. Rob Vanbergen will be speaking on Day 2 with a session titled What Is Microcurrent? How Home Use Microcurrent Can Help You Get Better Today.
In this talk, Dr. Rob will walk through what microcurrent therapy is, how it works, and how it may support inflammation reduction, tissue repair, nervous system regulation, and at-home pain relief. He will also share real-world healing examples and case studies, including how the vagus nerve can play a role in the healing process.
This conversation builds directly on the themes explored in this article: women deserve clearer answers, more comprehensive support, and practical tools to better understand what their bodies are asking for.
Save your spot for the Women’s Health Rescue Summit here.
Replays will be available.
Why nervous system regulation matters in women’s health
For many women, healing begins with the nervous system because it influences so much of what the body is able to do next. When the body spends too much time in fight-or-flight mode, sleep can become lighter or more disrupted, digestion may slow, recovery can take longer, and pain may feel more intense than it otherwise would.
This is why nervous system support matters in women’s health across life stages. Practices and therapies that help the body shift into a more settled, restorative state can create better conditions for healing, especially when stress, hormonal changes, inflammation, and chronic pain are all influencing one another.
Vagus nerve stimulation via microcurrent is one example. As the body begins to move out of a constant high-alert state, some women may feel more tired at first. That does not always mean something is wrong. In many cases, it may be a sign that the body finally feels safe enough to slow down and begin restoring the energy it has been borrowing for too long.
How stress and hormones affect women’s health across life stages

Many women carry years of emotional load in their bodies. Caregiving, trauma, overstimulation, grief, pressure to perform, and the habit of pushing through all take a toll. Over time, that burden can affect everything from pain levels to energy to immune function.
Hormones add another layer. Their shifts may show up as night sweats, feeling cold all the time, thinning hair, new acne, dry eyes, irritability, poor sleep, painful periods, worsening PMS, increased inflammation, or the sense that your body is responding differently than it used to.
Microcurrent is not a direct hormone replacement tool, but it can still be supportive. Many women use it to help with menopause symptom management, such as stress, brain fog, poor circulation, or nervous system overload. It can be one useful piece of the puzzle, even when it is not the whole answer.
How fascia and scar tissue affect women’s health
Fascia is one of the most overlooked aspects of women’s health, yet it influences far more than many people realize.
This connective tissue network surrounds muscles, bones, organs, nerves, and other structures throughout the body. When fascia becomes restricted through stress, injury, surgery, repetitive strain, or long-standing tension, those effects rarely stay confined to one area. They can influence posture, mobility, circulation, breath, and recovery in ways that are easy to miss when symptoms are assessed too narrowly.
For women, this matters in deeply practical ways. Pregnancy, birth, C-sections, hysterectomies, and other abdominal surgeries can leave behind scar tissue and adhesions that continue shaping the body long after initial recovery is considered complete.
A lingering C-section scar, for example, is not always just a mark on the surface. It may be associated with abdominal adhesions, pelvic tension, digestive changes, low back discomfort, or a lingering sense of tightness that never fully resolves. Some women also notice that after pregnancy or surgery, their abdominal wall no longer feels strong, coordinated, or well-supported. Over time, those changes can place more strain on the hips, pelvis, and lower back.
Stress and trauma can deepen those patterns even further. Many women carry protective tension in the abdomen, pelvis, diaphragm, and low back without realizing it. When that guarding becomes chronic, it can influence how the body moves, rests, breathes, and heals.
If this topic feels especially relevant to you, you may want to read our guide on using Microcurrent Therapy for Post-Surgical Healing.
This is also where lymphatic flow becomes important. When tissues are tight, irritated, or sluggish, women may feel puffy, heavy, inflamed, or slow to recover. Supporting fluid movement, circulation, and tissue health can make a meaningful difference.
For a deeper look at how fascia decompression can support pain relief, recovery, circulation, and detoxification, listen to Episode #53 of the Pain Free For Life podcast, featuring Deanna Hansen of Block Therapy.
And if post-surgical healing is part of your story, you may also want to explore the Post-Surgical Health Lab, where we dive deeper into non-invasive support for recovery, wound healing, inflammation, and scar care.
Frequently Asked Questions
Why can nervous system support make you feel tired at first?
When the body begins shifting out of chronic fight-or-flight and into a more restorative state, fatigue can become more noticeable. In many cases, it means the nervous system is no longer running on emergency energy, and the body is finally able to rest, repair, and recover more deeply.
Can microcurrent therapy help with hormone-related symptoms in women?
Microcurrent does not replace hormones or directly correct every hormonal imbalance, but it can help support many symptoms that often accompany hormonal shifts. Women may use microcurrent to support relaxation, circulation, menstrual comfort, brain fog, joint pain, nervous system regulation, and recovery, especially when those symptoms are made worse by stress, inflammation, or poor sleep. For a deeper look at how microcurrent fits into this broader picture, readers can start with our team’s women’s health roundtable discussion here.
How can scar tissue and fascia cause pain in other parts of the body?
Scar tissue and fascia can change how the body moves, stabilizes, and compensates. When tissue becomes restricted after surgery, injury, or long-standing tension, that strain can affect posture, mobility, circulation, and pain patterns elsewhere in the body. This is one reason a scar in the abdomen or pelvis can sometimes contribute to discomfort in the low back, hips, or ribcage.
What can women do first when they feel overwhelmed by symptoms?
A helpful first step is to slow down and look for patterns. Notice how sleep, stress, your cycle, pain levels, digestion, and energy change over time. From there, supporting the nervous system, improving rest, staying hydrated, and addressing obvious sources of strain can provide a more stable foundation for healing.
How do stress, hormones, and fascia connect in women’s health?
Women’s health is deeply interconnected. Stress can affect the nervous system, sleep, inflammation, and recovery. Hormonal shifts can influence mood, energy, pain sensitivity, and resilience. Fascia and scar tissue can shape movement, circulation, and tension patterns throughout the body. When these systems are viewed together rather than separately, symptoms often make more sense, and support can become more effective.
Continue learning and supporting your health
Women’s health is complex, but that does not mean your symptoms are random, insignificant, or something you are supposed to push through simply. When stress, hormones, fascia, scar tissue, sleep, and nervous system regulation are all influencing one another, it makes sense that healing may require a wider lens and a more thoughtful kind of support.
If this article reflected something you have been feeling, let that be your reminder to take yourself seriously. Pay attention to patterns. Ask better questions. Seek support that looks at the whole person, not just one symptom at a time.
If you want to keep learning, we recommend starting with the related resources referenced throughout this article, especially if post-surgical healing, scar tissue, or lingering tension patterns are part of your story. You can also explore the full range of microcurrent devices, wellness technologies, and educational resources trusted by the Pain Free For Life team at TheSanaShop.com.
The Sana Shop brings together the tools we use and recommend to support nervous system regulation, recovery, circulation, and whole-body healing.
SOURCES CITED:
https://researchautism.org/audience/research/the-autism-dilemma-for-women-diagnosis/
https://womenshealth.obgyn.msu.edu/blog/overlooked-or-misdiagnosed-conditions-women




